Business Name: BeeHive Homes of Maple Grove
Address: 14901 Weaver Lake Rd, Maple Grove, MN 55311
Phone: (763) 310-8111
BeeHive Homes of Maple Grove
BeeHive Homes at Maple Grove is not a facility, it is a HOME where friends and family are welcome anytime! We are locally owned and operated, with a leadership team that has been serving older adults for over two decades. Our mission is to provide individualized care and attention to each of the seniors for whom we are entrusted to care. What sets us apart: care team members selected based on their passion to promote wellness, choice and safety; our dedication to know each resident on a personal level; specialized design that caters to people living with dementia. Caring for those with memory loss is ALL we do.
14901 Weaver Lake Rd, Maple Grove, MN 55311
Business Hours
Monday thru Sunday: 7:00am to 7:00pm
Facebook: https://www.facebook.com/BeeHiveMapleGrove
Families typically come to memory care after months, in some cases years, of concern in the house. A father who roams at sunset. A mother whose arthritis makes stairs treacherous and whose judgment is slipping. A partner who wishes to be client but hasn't slept a complete night in weeks. Safety ends memory care up being the hinge that whatever swings on. The objective is not to cover people in cotton and get rid of all risk. The objective is to develop a location where people living with Alzheimer's or other dementias can live with dignity, relocation freely, and remain as independent as possible without being hurt. Getting that balance right takes careful design, smart routines, and staff who can check out a space the way a veteran nurse checks out a chart.
What "safe" suggests when memory is changing
Safety in memory care is multi-dimensional. It touches physical space, everyday rhythms, medical oversight, psychological wellness, and social connection. A secure door matters, however so does a warm hi at 6 a.m. when a resident is awake and trying to find the kitchen they keep in mind. A fall alert sensing unit helps, however so does understanding that Mrs. H. is uneasy before lunch if she hasn't had a mid-morning walk. In assisted living settings that provide a dedicated memory care neighborhood, the very best outcomes originate from layering securities that minimize risk without removing choice.
I have strolled into neighborhoods that gleam however feel sterilized. Homeowners there frequently walk less, eat less, and speak less. I have actually likewise walked into neighborhoods where the floors show scuffs, the garden gate is locked, and the personnel talk with homeowners like next-door neighbors. Those places are not ideal, yet they have far fewer injuries and much more laughter. Safety is as much culture as it is hardware.
Two core truths that guide safe design
First, individuals with dementia keep their impulses to move, look for, and explore. Roaming is not an issue to get rid of, it is a habits to redirect. Second, sensory input drives comfort. Light, noise, scent, and temperature shift how steady or upset an individual feels. When those two truths guide area preparation and daily care, dangers drop.
A corridor that loops back to the day room welcomes exploration without dead ends. A private nook with a soft chair, a lamp, and a familiar quilt offers a nervous resident a landing location. Fragrances from a small baking program at 10 a.m. can settle a whole wing. Alternatively, a screeching alarm, a refined flooring that glares, or a congested television space can tilt the environment toward distress and accidents.
Lighting that follows the body's clock
Circadian lighting is more than a buzzword. For people dealing with dementia, sunshine direct exposure early in the day helps control sleep. It improves mood and can minimize sundowning, that late-afternoon period when agitation rises. Go for bright, indirect light in the early morning hours, preferably with real daylight from windows or skylights. Avoid harsh overheads that cast hard shadows, which can appear like holes or barriers. In the late afternoon, soften the lighting to signal night and rest.
One community I worked with replaced a bank of cool-white fluorescents with warm LED fixtures and included an early morning walk by the windows that neglect the yard. The modification was easy, the outcomes were not. Residents started falling asleep closer to 9 p.m. and over night wandering reduced. Nobody included medication; the environment did the work.
Kitchen safety without losing the convenience of food
Food is memory's anchor. The smell of coffee, the ritual of buttering toast, the noise of a pan on a stove, these are grounding. In numerous memory care wings, the primary industrial kitchen area stays behind the scenes, which is suitable for safety and sanitation. Yet a little, supervised family kitchen location in the dining room can be both safe and reassuring. Think induction cooktops that stay cool to the touch, locked drawers for knives, and a dishwashing machine with auto-latch. Homeowners can assist whisk eggs or roll cookie dough while staff control heat sources.
Adaptive utensils and dishware reduce spills and frustration. High-contrast plates, either solid red or blue depending on what the menu appears like, can improve consumption for people with visual processing changes. Weighted cups aid with tremblings. Hydration stations with clear pitchers and cups at eye level promote drinking without a personnel prompt. Dehydration is one of the quiet threats in senior living; it sneaks up and results in confusion, falls, and infections. Making water visible, not just available, is a safety intervention.
Behavior mapping and individualized care plans
Every resident arrives with a story. Past professions, family functions, habits, and fears matter. A retired instructor may react best to structured activities at foreseeable times. A night-shift nurse may look out at 4 a.m. and nap after lunch. Best care honors those patterns rather than trying to force everybody into a consistent schedule.
Behavior mapping is a simple tool: track when agitation spikes, when wandering boosts, when a resident refuses care, and what precedes those minutes. Over a week or two, patterns emerge. Maybe the resident becomes disappointed when two staff talk over them during a shower. Or the agitation begins after a late day nap. Adjust the routine, change the method, and threat drops. The most knowledgeable memory care groups do this intuitively. For newer teams, a whiteboard, a shared digital log, and a weekly huddle make it systematic.
Medication management intersects with habits carefully. Antipsychotics and sedatives can blunt distress in the short term, but they also increase fall threat and can cloud cognition. Great practice in elderly care prefers non-drug methods first: music customized to personal history, aromatherapy with familiar scents, a walk, a snack, a quiet area. When medications are needed, the prescriber, nurse, and family needs to review the plan consistently and aim for the most affordable reliable dose.
Staffing ratios matter, but presence matters more
Families typically request a number: How many personnel per resident? Numbers are a starting point, not a finish line. A daytime ratio of one care partner to 6 or eight citizens is common in devoted memory care settings, with greater staffing in the evenings when sundowning can take place. Night shifts may drop to one to 10 or twelve, supplemented by a roving nurse or med tech. However raw ratios can deceive. A skilled, constant group that knows homeowners well will keep individuals safer than a bigger but constantly altering group that does not.
Presence implies staff are where homeowners are. If everybody congregates near the activity table after lunch, a team member need to be there, not in the workplace. If three residents choose the peaceful lounge, established a chair for staff in that area, too. Visual scanning, soft engagement, and gentle redirection keep incidents from ending up being emergency situations. I as soon as enjoyed a care partner spot a resident who liked to pocket utensils. She handed him a basket of fabric napkins to fold instead. The hands stayed busy, the threat evaporated.
Training is similarly substantial. Memory care staff need to master techniques like favorable physical method, where you go into an individual's space from the front with your hand provided, or cued brushing for bathing. They need to understand that duplicating a question is a search for peace of mind, not a test of persistence. They ought to understand when to go back to reduce escalation, and how to coach a relative to do the same.
Fall prevention that respects mobility
The best way to trigger deconditioning and more falls is to dissuade walking. The much safer course is to make walking much easier. That begins with shoes. Motivate families to bring tough, closed-back shoes with non-slip soles. Prevent floppy slippers and high heels, no matter how cherished. Gait belts work for transfers, however they are not a leash, and homeowners ought to never ever feel tethered.
Furniture ought to invite safe movement. Chairs with arms at the right height assistance homeowners stand independently. Low, soft couches that sink the hips make standing hazardous. Tables need to be heavy enough that citizens can not lean on them and move them away. Hallways take advantage of visual cues: a landscape mural, a shadow box outside each space with individual photos, a color accent at space doors. Those cues lower confusion, which in turn decreases pacing and the hurrying that results in falls.
Assistive technology can help when picked attentively. Passive bed sensing units that inform staff when a high-fall-risk resident is getting up decrease injuries, particularly at night. Motion-activated lights under the bed guide a safe course to the restroom. Wearable pendants are a choice, however many people with dementia eliminate them or forget to push. Innovation needs to never ever substitute for human presence, it ought to back it up.
Secure perimeters and the ethics of freedom
Elopement, when a resident exits a safe location unnoticed, is amongst the most feared occasions in senior care. The action in memory care is safe and secure perimeters: keypad exits, postponed egress doors, fence-enclosed courtyards, and sensor-based alarms. These functions are warranted when utilized to prevent risk, not restrict for convenience.
The ethical concern is how to protect flexibility within required boundaries. Part of the answer is scale. If the memory care area is big enough for locals to stroll, find a quiet corner, or circle a garden, the restriction of the external boundary feels less like confinement. Another part is purpose. Offer reasons to remain: a schedule of significant activities, spontaneous chats, familiar jobs like arranging mail or setting tables, and disorganized time with safe things to play with. People walk towards interest and away from boredom.
Family education assists here. A child might balk at a keypad, remembering his father as a Navy officer who could go anywhere. A considerate discussion about risk, and an invite to sign up with a courtyard walk, frequently moves the frame. Liberty includes the freedom to stroll without fear of traffic or getting lost, which is what a safe border provides.
Infection control that does not remove home
The pandemic years taught hard lessons. Infection control belongs to security, however a sterilized environment hurts cognition and mood. Balance is possible. Usage soap and warm water over constant alcohol sanitizer in high-touch areas, because broken hands make care undesirable. Choose wipeable chair arms and table surface areas, but avoid plastic covers that squeak and stick. Preserve ventilation and usage portable HEPA filters quietly. Teach staff to use masks when indicated without turning their faces into blank slates. A smile in the eyes, a name badge with a large picture, and the habit of stating your name first keeps heat in the room.
Laundry is a quiet vector. Residents often touch, smell, and carry clothing and linens, specifically products with strong personal associations. Label clothes clearly, wash consistently at appropriate temperatures, and manage stained items with gloves but without drama. Calmness is contagious.
Emergencies: planning for the unusual day
Most days in a memory care neighborhood follow foreseeable rhythms. The uncommon days test preparation. A power blackout, a burst pipeline, a wildfire evacuation, or a serious snowstorm can turn safety upside down. Communities ought to maintain composed, practiced plans that represent cognitive impairment. That consists of go-bags with standard materials for each resident, portable medical details cards, a staff phone tree, and developed shared help with sis communities or local assisted living partners. Practice matters. A once-a-year drill that actually moves citizens, even if just to the yard or to a bus, exposes spaces and develops muscle memory.
Pain management is another emergency situation in slow motion. Neglected pain provides as agitation, calling out, withstanding care, or withdrawing. For people who can not name their pain, personnel should use observational tools and understand the resident's baseline. A hip fracture can follow a week of hurt, hurried strolling that everyone mistook for "uneasyness." Safe neighborhoods take discomfort seriously and intensify early.
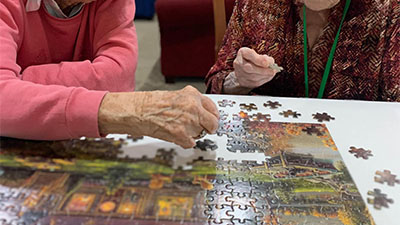

Family partnership that strengthens safety
Families bring history and insight no evaluation type can capture. A daughter may understand that her mother hums hymns when she is content, or that her father relaxes with the feel of a newspaper even if he no longer reads it. Welcome families to share these information. Construct a short, living profile for each resident: preferred name, pastimes, previous occupation, preferred foods, activates to prevent, soothing regimens. Keep it at the point of care, not buried in a chart.
Visitation policies should support involvement without frustrating the environment. Motivate family to sign up with a meal, to take a yard walk, or to help with a favorite task. Coach them on method: greet gradually, keep sentences basic, avoid quizzing memory. When households mirror the staff's techniques, homeowners feel a stable world, and safety follows.
Respite care as a step toward the best fit
Not every family is all set for a complete transition to senior living. Respite care, a short remain in a memory care program, can provide caregivers a much-needed break and provide a trial duration for the resident. Throughout respite, personnel learn the person's rhythms, medications can be reviewed, and the family can observe whether the environment feels right. I have seen a three-week respite expose that a resident who never napped in your home sleeps deeply after lunch in the community, just since the morning consisted of a safe walk, a group activity, and a well balanced meal.
For families on the fence, respite care lowers the stakes and the tension. It also surfaces practical questions: How does the neighborhood manage restroom cues? Are there enough peaceful areas? What does the late afternoon appear like? Those are security concerns in disguise.
Dementia-friendly activities that decrease risk
Activities are not filler. They are a main security method. A calendar packed with crafts but absent movement is a fall threat later on in the day. A schedule that rotates seated and standing tasks, that includes purposeful tasks, which appreciates attention period is more secure. Music programs are worthy of unique reference. Years of research and lived experience reveal that familiar music can decrease agitation, improve gait consistency, and lift mood. An easy ten-minute playlist before a tough care minute like a shower can change everything.
For locals with sophisticated dementia, sensory-based activities work best. A basket with material examples, a box of smooth stones, a warm towel from a small towel warmer, these are relaxing and safe. For citizens previously in their illness, assisted walks, light stretching, and simple cooking or gardening provide significance and movement. Security appears when individuals are engaged, not just when dangers are removed.
The role of assisted living and when memory care is necessary
Many assisted living communities support homeowners with moderate cognitive problems or early dementia within a wider population. With great staff training and ecological tweaks, this can work well for a time. Indications that a dedicated memory care setting is more secure consist of consistent wandering, exit-seeking, inability to utilize a call system, frequent nighttime wakefulness, or resistance to care that escalates. In a mixed-setting assisted living environment, those needs can stretch the staff thin and leave the resident at risk.
Memory care communities are constructed for these realities. They normally have secured gain access to, higher staffing ratios, and spaces tailored for cueing and de-escalation. The decision to move is seldom easy, however when security ends up being a daily concern in your home or in general assisted living, a transition to memory care typically restores stability. Families often report a paradox: once the environment is more secure, they can return to being partner or kid rather of full-time guard. Relationships soften, which is a sort of safety too.
When risk is part of dignity
No community can remove all risk, nor must it try. Absolutely no danger often indicates absolutely no autonomy. A resident might wish to water plants, which brings a slip risk. Another might demand shaving himself, which carries a nick risk. These are appropriate risks when supported thoughtfully. The doctrine of "self-respect of threat" acknowledges that grownups keep the right to make choices that bring consequences. In memory care, the team's work is to understand the individual's worths, involve family, put affordable safeguards in place, and display closely.
I remember Mr. B., a carpenter who enjoyed tools. He would gravitate to any drawer pull or loose screw in the structure. The knee-jerk action was to get rid of all tools from his reach. Rather, personnel developed a monitored "workbench" with sanded wood blocks, a hand drill with the bit removed, and a tray of washers and bolts that might be screwed onto an installed plate. He invested delighted hours there, and his urge to dismantle the dining room chairs disappeared. Threat, reframed, became safety.
Practical indications of a safe memory care community
When touring communities for senior care, look beyond pamphlets. Invest an hour, or 2 if you can. Notice how personnel speak with homeowners. Do they crouch to eye level, usage names, and wait for actions? See traffic patterns. Are citizens gathered together and engaged, or drifting with little direction? Look into restrooms for grab bars, into hallways for handrails, into the courtyard for shade and seating. Sniff the air. Clean does not smell like bleach throughout the day. Ask how they manage a resident who tries to leave or refuses a shower. Listen for considerate, specific answers.

A couple of concise checks can help:
- Ask about how they lower falls without reducing walking. Listen for information on flooring, lighting, shoes, and supervision. Ask what occurs at 4 p.m. If they describe a rhythm of calming activities, softer lighting, and staffing presence, they understand sundowning. Ask about staff training particular to dementia and how often it is revitalized. Yearly check-the-box is not enough; search for continuous coaching. Ask for examples of how they customized care to a resident's history. Specific stories signal real person-centered practice. Ask how they communicate with households everyday. Websites and newsletters help, however fast texts or calls after significant occasions develop trust.
These concerns reveal whether policies live in practice.
The peaceful infrastructure: documents, audits, and continuous improvement
Safety is a living system, not a one-time setup. Communities should investigate falls and near misses, not to designate blame, however to learn. Were call lights answered immediately? Was the flooring damp? Did the resident's shoes fit? Did lighting modification with the seasons? Existed staffing spaces during shift change? A short, focused evaluation after an occurrence frequently produces a little repair that prevents the next one.
Care plans need to breathe. After a urinary system infection, a resident may be more frail for a number of weeks. After a family visit that stirred feelings, sleep may be interfered with. Weekly or biweekly team gathers keep the strategy existing. The very best groups record little observations: "Mr. S. drank more when used warm lemon water," or "Ms. L. steadied better with the green walker than the red one." Those details build up into safety.
Regulation can assist when it demands significant practices rather than paperwork. State rules vary, however a lot of require safe boundaries to fulfill specific standards, personnel to be trained in dementia care, and event reporting. Neighborhoods need to fulfill or go beyond these, but families should likewise examine the intangibles: the steadiness in the building, the ease in locals' faces, the way staff move without rushing.
Cost, value, and hard choices
Memory care is expensive. Depending on region, monthly costs range extensively, with private suites in metropolitan areas often significantly greater than shared rooms in smaller sized markets. Households weigh this versus the cost of employing in-home care, modifying a house, and the personal toll on caretakers. Safety gains in a well-run memory care program can decrease hospitalizations, which carry their own expenses and dangers for elders. Avoiding one hip fracture avoids surgical treatment, rehabilitation, and a cascade of decline. Preventing one medication-induced fall preserves mobility. These are unglamorous savings, however they are real.
Communities sometimes layer pricing for care levels. Ask what activates a shift to a higher level, how roaming behaviors are billed, and what takes place if two-person help becomes necessary. Clearness avoids difficult surprises. If funds are limited, respite care or adult day programs can postpone full-time positioning and still bring structure and safety a couple of days a week. Some assisted living settings have monetary counselors who can help families explore advantages or long-lasting care insurance policies.
The heart of safe memory care
Safety is not a checklist. It is the feeling a resident has when they reach for a hand and discover it, the predictability of a favorite chair near the window, the understanding that if they get up during the night, someone will observe and fulfill them with kindness. It is likewise the confidence a son feels when he leaves after supper and does not sit in his vehicle in the car park for twenty minutes, fretting about the next telephone call. When physical design, staffing, regimens, and family partnership align, memory care ends up being not simply more secure, but more human.
Across senior living, from assisted living to devoted memory neighborhoods to short-stay respite care, the communities that do this best reward security as a culture of listening. They accept that threat belongs to real life. They counter it with thoughtful design, constant people, and meaningful days. That combination lets homeowners keep moving, keep picking, and keep being themselves for as long as possible.
BeeHive Homes of Maple Grove provides assisted living care
BeeHive Homes of Maple Grove provides memory care services
BeeHive Homes of Maple Grove is a memory care home for seniors
BeeHive Homes of Maple Grove provides respite care services
BeeHive Homes of Maple Grove offers 24-hour support from professional caregivers
BeeHive Homes of Maple Grove offers private bedrooms with private bathrooms
BeeHive Homes of Maple Grove provides medication monitoring and documentation
BeeHive Homes of Maple Grove serves dietitian-approved meals
BeeHive Homes of Maple Grove provides housekeeping services
BeeHive Homes of Maple Grove provides laundry services
BeeHive Homes of Maple Grove offers community dining and social engagement activities
BeeHive Homes of Maple Grove features life enrichment activities
BeeHive Homes of Maple Grove supports personal care assistance during meals and daily routines
BeeHive Homes of Maple Grove promotes frequent physical and mental exercise opportunities
BeeHive Homes of Maple Grove provides a home-like residential environment
BeeHive Homes of Maple Grove creates customized care plans as residents’ needs change
BeeHive Homes of Maple Grove assesses individual resident care needs
BeeHive Homes of Maple Grove accepts private pay and long-term care insurance
BeeHive Homes of Maple Grove assists qualified veterans with Aid and Attendance benefits
BeeHive Homes of Maple Grove encourages meaningful resident-to-staff relationships
BeeHive Homes of Maple Grove delivers compassionate, attentive senior care focused on dignity and comfort
BeeHive Homes of Maple Grove has a phone number of (763) 310-8111
BeeHive Homes of Maple Grove has an address of 14901 Weaver Lake Rd, Maple Grove, MN 55311
BeeHive Homes of Maple Grove has a website https://beehivehomes.com/locations/maple-grove/
BeeHive Homes of Maple Grove has Google Maps listing https://maps.app.goo.gl/n99VhHgdH879gqTH8
BeeHive Homes of Maple Grove has Facebook page https://www.facebook.com/BeeHiveMapleGrove
BeeHive Homes of Maple Grove won Top Memory Care Homes 2025
BeeHive Homes of Maple Grove earned Best Customer Service Award 2024
BeeHive Homes of Maple Grove placed 1st for Senior Living Memory Care Communities 2025
People Also Ask about BeeHive Homes of Maple Grove
What is BeeHive Homes of Maple Grove monthly room rate?
The rate depends on the level of care that is needed. We do an initial evaluation for each potential resident to determine the level of care needed. The monthly rate is based on this evaluation. There are no hidden costs or fees
Can residents stay in BeeHive Homes of Maple Grove until the end of their life?
Usually yes. There are exceptions, such as when there are safety issues with the resident, or they need 24 hour skilled nursing services
Does BeeHive Homes of Maple Grove have a nurse on staff?
Yes. We have a team of four Registered Nurses and their typical schedule is Monday - Friday 7:00 am - 6:00 pm and weekends 9:00 am - 5:30 pm. A Registered Nurse is on call after hours
What are BeeHive Homes of Maple Grove's visiting hours?
Visitors are welcome anytime, but we encourage avoiding the scheduled meal times 8:00 AM, 11:30 AM, and 4:30 PM
Where is BeeHive Homes of Maple Grove located?
BeeHive Homes of Maple Grove is conveniently located at 14901 Weaver Lake Rd, Maple Grove, MN 55311. You can easily find directions on Google Maps or call at (763) 310-8111 Monday through Sunday 7am to 7pm.
How can I contact BeeHive Homes of Maple Grove?
You can contact BeeHive Homes of Maple Grove by phone at: (763) 310-8111, visit their website at https://beehivehomes.com/locations/maple-grove, or connect on social media via Facebook
Weaver Lake Community Park provides a serene lakeside walk perfect for assisted living and memory care residents to enjoy fresh air and gentle scenery during senior care and respite care outings.